Medicaid managed care plans recognize the effects of social determinants of health—non-medical factors that nonetheless have lasting impacts on health, wealth, and wellness—and are tackling them head on to provide better care. These factors include where and how we live, work, and play – and can determine up to 60 percent of our overall health.
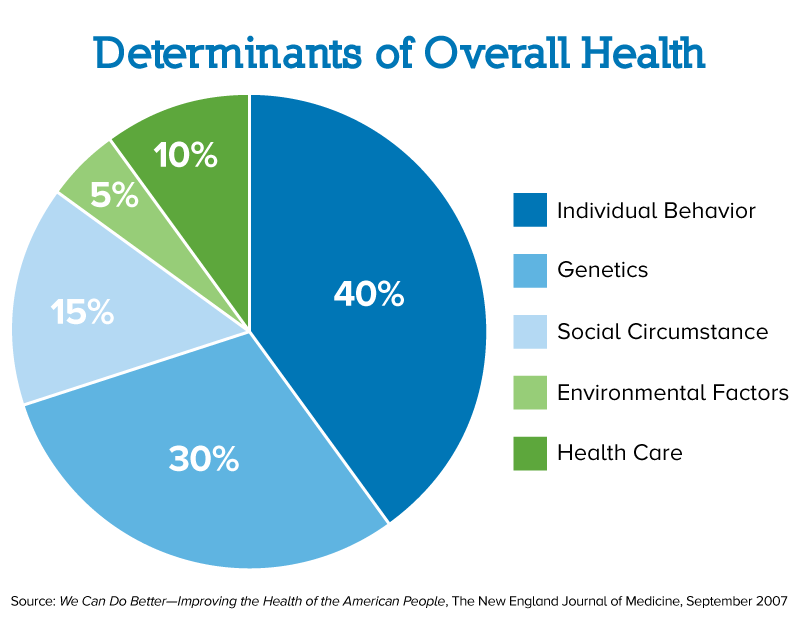
Medicaid plans are taking innovative approaches to keep people healthy and address the outsize impact of social determinants of health. Below are two examples of their work.
Cultivating Health for Success: A partnership between UPMC Health Plans and Community Human Services, the program integrates housing, an assigned medical home, case management, and care coordination to provide housing stability for members. Medical costs and unplanned care have declined among homeless individuals who gained stable housing through the program since 2010. Participants who gained housing also saw an average annual health savings of $6,384.
Life Services JobConnect: A pilot program in Ohio, Indiana, and Georgia, Life Services JobConnect is designed to help people get and keep jobs that can improve their lives. The program helps connect members with employers and improve their long-term financial stability. It also provides services we all need to help us get and keep jobs, like stress management, transportation, childcare, and personal finance classes. Through JobConnect, members are able to access a pathway out of poverty and into a successful career.
These programs, and many others like them, are directly addressing social determinants of health. By tackling the non-medical factors of health, Medicaid plans are improving the health of their members and advancing health equity – and that’s something that makes life better for all of us.