Modern Medicaid Alliance (MMA): What role have nurse practitioners played in the nationwide COVID-19 vaccination effort?

April Kapu (AANP): There are currently 325,000 NPs practicing in the United States representing nearly every geographic region and health care setting in the country. They have been integral in educating their patients on the importance of receiving their COVID-19 vaccine and administering the vaccine. According to an AANP member survey conducted in Spring of 2021, approximately a quarter reported administering vaccines, with about half reporting that they will be able to do so once the vaccine is available in their practice settings.
MMA: How have nurse practitioners provided care for underserved communities and helped them meet their immunization needs?

AANP: NPs are most likely to be present in rural and underserved communities. Individuals in such communities are less likely to have a regular source of health care, more likely to be vaccine hesitant and experience more logistical issues in accessing the vaccines that complicate the process of becoming vaccinated. NPs have been working in these communities to address issues of access and hesitancy. One of the other major concerns of this pandemic is that to avoid exposure to infections, patients have been reluctant to receive non-COVID care particularly routine vaccinations and treatment for mental health conditions and substance use disorders. All of these issues are exacerbated in underserved communities. NPs have been working to ensure that underserved communities are able to meet their health care needs through telehealth, at-home visits and by modifying their clinics to ensure patient safety.
MMA: How effective has the recent vaccine-focused work of nurse practitioners been to overcoming health disparities?
AANP: NPs have been part of an “all-hands on deck” approach to overcome health disparities as it relates to vaccines. A May 21, 2021 Morbidity and Mortality Weekly Report (MMWR) published by the CDC stated that “86% of rural residents report they trust their own health care providers for information on COVID-19 vaccines.” Using their voice as trusted health care providers, NPs have been involved with efforts to encourage vaccinations and increase vaccine confidence, especially in hesitant communities. For example, NPs are the most common provider in community health centers, so they were vital when the Administration focused on increasing vaccinations within those settings. While there is still a lot of work to be done, we have seen increasing vaccination rates and surveys showing decreases in vaccine hesitancy which indicate that the work of all parties, NPs included, is having a positive impact on vaccination rates in underserved communities.
MMA: In what ways has the COVID-19 pandemic impacted NP clinical practice across settings and specialties? 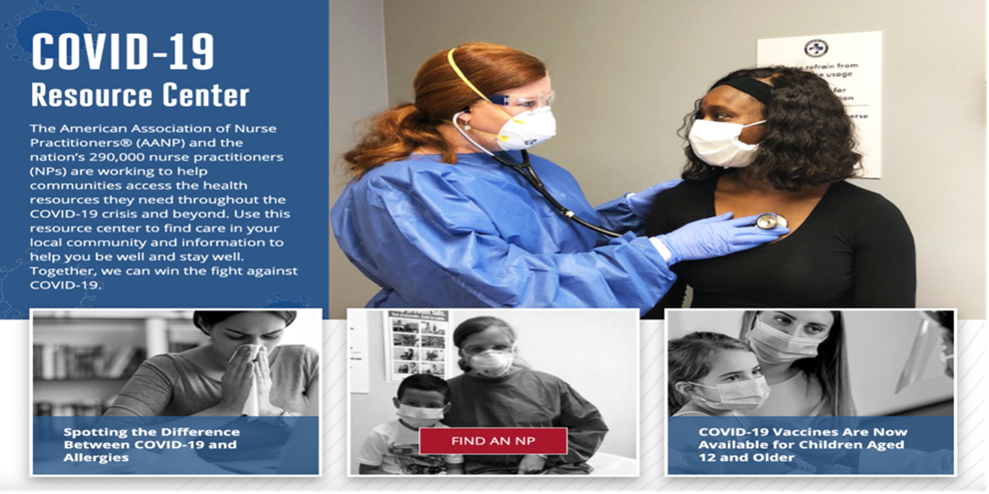
AANP: The experiences have varied depending on the geographic area, practice setting and stage of the pandemic. Particularly early in the pandemic, NPs in areas that had not yet experienced a COVID-19 surge often experienced decreases in patient visits that led to layoffs and furloughs of NPs and other clinical staff. However, in other locations, NPs were preparing for patient surges and were being moved throughout facilities and settings into the highest-need areas. Recognizing the important impact of nurse practitioners on the COVID-19 response, states and the federal government have waived many barriers that prevented them from practicing to the full extent of their education and clinical training. These actions have been important to improving health care access, reducing patient exposure to COVID-19 and maximizing the impact of our clinical workforce. It is important that waivers issued by the U.S. Department of Health and Human Services and state governments are made permanent to provide better overall care for patients.
MMA: How has telehealth improved nurse practitioner ability to reach patients? 
AANP: NPs quickly started or expanded the telehealth services that they provide to patients and have reported the important impact of telehealth on reaching patients in need to treatment. The increased telehealth coverage and removal of certain barriers and restrictions has been an essential lifeline for NPs to meet the needs of their patients. NPs have shown an overwhelming transition to the use of telehealth to prevent the spread of COVID-19 and have pioneered new methods to meet the health care needs of their patients. Increased reimbursement for audio-only services has also been imperative to treating underserved communities, where many patients have difficulty accessing broadband or audio-visual telehealth modalities. These include patients without synchronized two-way audio-visual technology in their homes, and those in areas without access to the necessary internet and broadband capabilities needed to support these interactions. Coverage of audio-only services will be critical moving forward to ensure equitable access to care.
MMA: Have you engaged with Medicaid beneficiaries in unique ways around vaccinations and if yes, how?
AANP: Many of the previously mentioned efforts in which our members have engaged (community health centers for example), are primarily focused on serving Medicaid beneficiaries and uninsured or underinsured individuals. AANP has also created patient-facing website, WeChooseNPs.org, which provides patient-focused information. The organization is also a member of several coalitions focused on increasing vaccinations in underserved communities such as the HHS Community Corps, Made to Save and the COVID-19 Vaccine Education and Equity Project which have all done great work to educate patients on the vaccine and engage local communities.